Gastroscopy is the endoscopic examination of the upper gastrointestinal tract by means of a flexible fiberoptic endoscope, that is enable the doctor to look inside of the esophagus, stomach, and duodenum. This device has a length of approximately 1200 mm and diameter of approx. 10 mm. The instrument shaft is composed of numerous specialized glass fibers which allow the transmission of light down the length thin fiber with minimal distortion. The multiple optic images are integrated at the proximal unit, by means of a complex system of lenses. The endoscopist thus views a reconstructed, mosaic image at the proximal eyepiece (similar to a television image). Also within the instrument shaft are several channels designated for passage of optional devices such as biopsy forceps, polyp snare, cautery, and suction. Air may also be introduced for insufflations of the stomach. For clearing of debris from the viewing area, a jet stream of water from separate reservoir can be flushed through one channel.
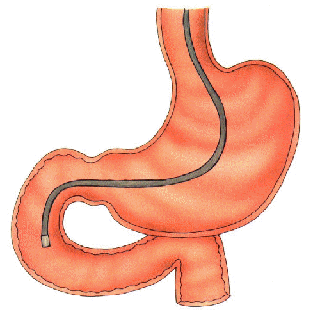
Reason for procedure
Indications for gastroscopy include:
• Upper gastrointestinal bleeding , to establish the exact location of hemorrhage
• Dysphagia
• Dyspepsia, if refractory to standard medical treatment
• Unexplained upper abdominal pain, dyscomfort
• Atypical chest pain
• Acid regurgitation, heartburn
• Lack of appetite
• Loss of weight
• Surveillance endoscopy fro known pre-malignant conditions, such as Barrett’s esophagus, severe chronic atrophic gastritis
• Abnormalities which require visual confirmation and tissue biopsy (eg, polyps, gastric ulcer, strictures).
What happens during gastroscopy?
Gastroscopy requires proper preparation. The results from gastroscopy are dependent on the stomach being empty. The stomach has to be completely clean, that means the patient should not eat 4-5 hours before the examination. Food particles inside the stomach may increase the risk of aspiration during the examination and can hide important conditions that may be present. The examination is performed only by an experienced gastroenterologist in a properly equipped endoscopy unit. A hollow mouthpiece is inserted to protect the patient’s teeth and facilitate instrument passage. Patient is placed in the left lateral decubitus position. For making the insertion of the instrument easier, local anesthetic is used. If it is requested or necessary the patient can receive intravenous sedation. The endoscope is slowly advanced orally and is “swallowed” by the patient. Once past the cricopharyngeal region the instrument is guided only under direct visualization. The instrument is inserted into the esophagus, than various portions of the stomach are inspected. Following thus, the endoscope is than passed through the pylorus, into the duodenum. Mucosal surfaces are re-inspected as the instrument is withdrawn. Biopsies, polypectomy, cauterization of bleeding lesions, are performed as indicated.
During endoscopy small mucosa samples with biopsy forceps should be taken. The biopsy samples will be tested by histology for the existence Helicobacter pylori, inflammation or gastric cancer. Helicobacter pylori is a bacterium in the stomach which can cause chronic gastritis, peptic ulcer and sometimes gastric cancer. Once gastric polyps are removed, they can be studied with the aid of a microscope to determine if they are precancerous or not.
The examination is done as an outpatient procedure and will only take some minutes. The patient is able to perform normal daily activities afterwards. Only if intravenous sedation was administered, the patient should take a short rest. The patient should not drive or operate machinery afterwards.
 Magyar
Magyar